 Protest at a Madrid hospital. | María Álvarez del Vayo
Protest at a Madrid hospital. | María Álvarez del Vayo
COVID-19 pandemic exposes southern Europe’s nursing shortage
For weeks, Spain and Italy were epicentres of the COVID-19 pandemic. Their health defences had an important gap.
Every evening this spring, when the clocks struck eight, thousands of people across Europe came out to applaud from their balconies. They did this to recognise the immense effort of healthcare workers who are still fighting to save the lives of thousands of patients. Since the crisis began, Europe has recorded over 1.5 million cases. COVID-19 has killed at least 174,000 Europeans.
“These have been very hard months. What health centres have experienced is appalling,” says María José García, spokesperson for SATSE, the main Spanish nursing union. García, who works in Madrid, has been one of thousands of healthcare workers who have been on the front line against the virus. As in other European countries, they have made a titanic effort despite the lack of resources.
However, there is an invisible line across Europe. Before COVID-19 hit, the Nordic and Central European countries had the best prepared health staff. Although the number of doctors per capita was similar to southern Europe, another important link in the chain differed: nursing. The northern and central European countries had many more nurses than did southern European countries. According to Eurostat data, Germany had almost 13 nurses per thousand inhabitants, similar to Luxembourg (11.72), Belgium (10.96), Sweden (10.90), the Netherlands (10.88) or Denmark (9.95).
At the other extreme, Greece had 3.31 nurses per thousand inhabitants in 2017, the lowest number. According to Eurostat data, other southern countries also had large staffing shortages. Spain, with 5.74 nursing specialists per thousand inhabitants, and Italy, with 5.80, were far more short-handed than their northern neighbours. During the height of the pandemic, both Spain and Italy became epicentres of the health crisis. The COVID-19 emergency has revealed, more clearly than ever, one of the historical weaknesses of those countries’ health systems: the nursing shortage. The fewer the nurses per patient the worse the health outcomes, according to a study of 300 hospitals in nine European countries.
Italy and Spain also have lower than average ratios of nurses to doctors. In general, the Nordic and Central European countries have close to the Organisation for Economic Cooperation and Development (OECD) average of three nurses for each doctor. In contrast, Italy had 1.45 and in Spain the ratio was similar: 1.48. This is because the number of doctors in both countries are similar to the European average, unlike the number of nurses, of whom there are far fewer in southern European countries.
“Our healthcare system focuses more on curing than caring for people or preventing disease,” explains Mar Rocha, spokesperson for the Official College of Nursing of Madrid (CODEM, in Spanish).
The situation is even worse in care homes.
“Care homes for dependent people, not just for the elderly, have always had a very poor ratio,” Rocha says. “If historically in the health field there are few nurses, in the social health field we are practically alone. This pandemic has made that lack of healthcare visible and has wreaked havoc on residents,” she says. As of June 10, about 20,000 residents of Spanish nursing homes had died of COVID-19 or with its symptoms.
Different data for the same reality
The data included corresponds to practising healthcare personnel, the Eurostat category that includes both doctors and nurses, who “directly care for patients.” However, some European countries, such as France, Portugal, Ireland and Slovakia, do not disclose their figures in this category. The data they publish in their national reports are for “active professionals,” a slightly different category, which includes not only working professionals but all license holders. While not directly comparable and therefore excluded from our table, France and Portugal had higher proportions of nurses than Spain and Italy: in 2018, the French health system had 10.48 nurses per 1000 inhabitants, while the Portuguese system had 7.2. We excluded Romania, Czechia and Greece due to problems in their numbers of doctors or nurses. We explain in the methodology section at the end of this article peculiarities in other countries’ healthcare workers reporting.
“There is an endemic lack of nurses,” says García, the Spanish nursing union spokesperson.
Barbara Mangiacavalli, president of the National Federation of Nursing Professionals (FNOPI) says it is the same in Italy. The Italian Court of Auditors wrote in a recent report that lower public spending on Italian healthcare has led to fewer healthcare personnel working the country, especially nurses. Italy would need to add between 53,000 and 54,000 nurses to reach the European average proportion of nurses in the population, according to FNOPI. In Spain, the shortage is between 88,000 and 125,000 nurses, according to the Spanish nursing union, SATSE, and Madrid official college of nursing, CODEM. The OECD has also highlighted the nursing shortage in both countries.
“Historically, nurses have had very little visibility,” says Rocha, the spokesperson for the Madrid official college of nursing, which “translates into a lack of social recognition.”
“Most people think of us as staff under the orders of doctors in hospitals and health centres, but that is not the case,” García says.
Nurses lead patient care and are in direct contact with them on an ongoing basis, Rocha says. Their work during the COVID-19 pandemic has multiplied exponentially.
“Beyond healthcare, our role was to never leave any patient alone,” Mangiacavalli says.
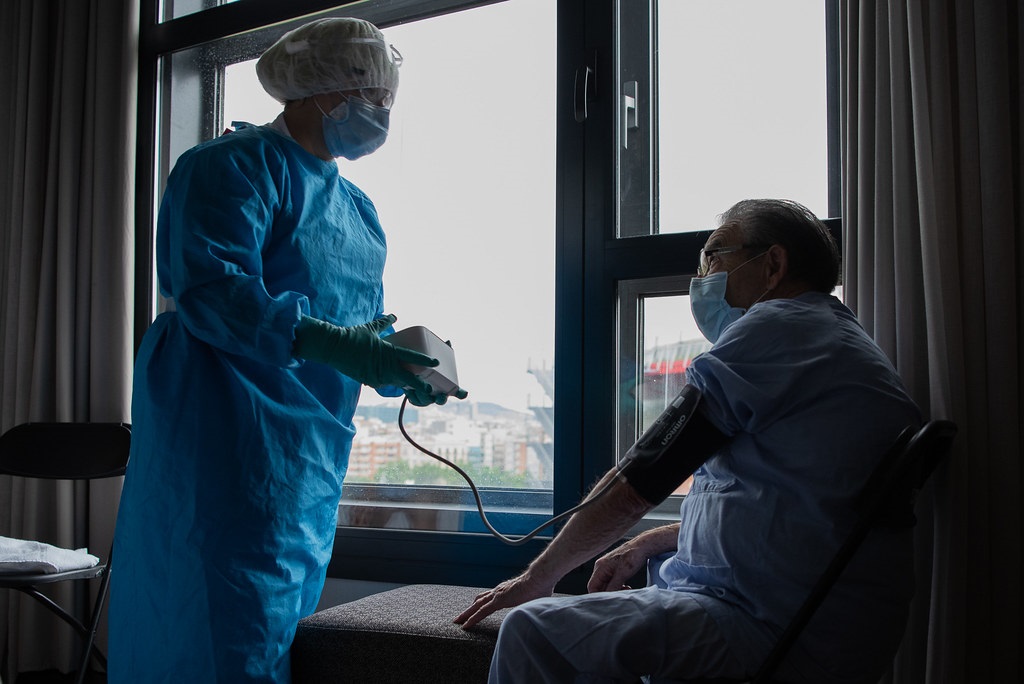
Hospital Clínic | Flickr
Healthcare workers in the breach
That explains why nurses, like other healthcare workers, had higher infection rates than the general population. In early April, the World Health Organization warned that 10% of all infections in the European region were healthcare workers. Soon after, in late April, the European Centres for Disease Prevention and Control (ECDC) published some revealing figures: 20% of people with COVID-19 in Spain were healthcare workers. In Italy the percentage was 10%, although in some of the most affected areas, such as Lombardy, the proportion of infected healthcare workers reached 20%.
Because healthcare workers are overwhelmingly women, women are suffering higher rates of COVID-19 than they otherwise would. At the beginning of June, 70% of Italian healthcare workers with COVID-19 were women, the Istituto Superiore di Sanità reports. Similarly, 76% of Spanish healthcare workers with COVID-19 were women. But only 56% of the general population in Spain with COVID-19 were women. Why the difference? According to Eurostat, 78% of all healthcare workers are women, and the ratio is even higher in nursing. “It has been a highly feminised profession since its origin,” Rocha says.
“I have never known a fireman who goes into a burning house without protection, but the governments asked nurses to go into the COVID units without any protection and to risk their lives”
Policymakers have offered several explanations for the higher rate of infection among healthcare workers. In Spain, for example, the Health Ministry attributed it to the higher diagnostic testing rates among healthcare workers, greater exposure to the virus at work and the initial ignorance about asymptomatic transmission. However, they do not mention the problem that professional organisations claim caused the infections: the lack of personal protective equipment.
“We are not heroes, we do not wear capes nor do we have superpowers. That is why we have the infection rate that we have,” García says. According to a recent study in Spain, during the first weeks of the epidemic, healthcare workers especially noted the lack of availability of filter masks, for example, to protect themselves, both in hospitals and in primary care.
“I have never known a fireman who goes into a burning house without protection, but the governments asked nurses to go into the COVID units without any protection and to risk their lives. This is unacceptable,” says Paul De Raeve, secretary general of the European Federation of Nursing Associations (EFN).
As of May 29, 51,482 Spanish healthcare professionals had been infected with coronavirus.
The same thing happened in Italy. According to FNOPI data, some 13,000 Italian nurses were infected with COVID-19, almost half of the 30,000 healthcare workers infected in this country.
“Forty died of COVID-19, and this despite the fact that the nursing population is young enough to better withstand the effects of the virus,” says Mangiacavalli, the Italian nursing association president. But what happened with COVID-19, as de Raeve says, is nothing new. When Ebola first came to Europe in 2014, a health worker caught the dangerous virus in a Madrid hospital. Back then, healthcare professional associations and unions focused on the need for personal protective equipment.
“Nobody paid any attention,” de Raeve recalls. Now, the International Council of Nursing (ICN), calls the situation a “global emergency.” As of May 18, according to an ICN letter to the World Health Organization, at least 360 nurses worldwide had died of COVID-19. However, many countries, including Spain, do not break down data by professional categories, so this figure could just be the tip of the iceberg.
“We need to make sure that we take care of those who care for us,” de Raeve says.

Protest at a Madrid hospital | María Álvarez del Vayo
The invisible footprint
The impact of COVID-19 worldwide has been and will continue to be enormous. But for frontline staff, it may be even greater. The emotional overload and the feeling of lack of protection soon added to the enormous amount of pandemic-related work. Garcia says, “You go to work afraid of infecting your family, of becoming a vector for the disease.”
“When you have thirty years of professional experience, many people have died throughout your life and you get used to it. But you know how to deal with it because it only happens from time to time,” García adds. But COVID-19 crisis became an unmanageable nightmare overnight. Patients died almost continuously, in most cases alone and far from their families.
“We are continually exposed to people’s pain and illness, but this crisis has been an emotional and psychological tsunami,” Rocha says. In fact, preliminary research from the Complutense University of Madrid shows how almost 80% of the healthcare workers interviewed had symptoms of anxiety and 51% suffered signs related to depression. Rocha and García both told Civio of endless hours of work, of hundreds of patients to look after, of the urgency and of the distressing number of dead they saw every day. Despite the physical and mental fatigue, their commitment was unequivocal: “Never leave anyone alone,” Mangiacavalli says.

Hospital Clínic | Flickr
For De Raeve, that mission and the will to complete it reflects the commitment of the nursing profesion, which is commemorating its international year in 2020. Few imagined at the start of this year that it would take place in the midst of a global pandemic that would shine a light on the value of nursing. Yet nurses suffer high levels of job insecurity, he says: in Spain, work contracts sometimes last just weeks or even days. In Italy, salaries are far below the European average. According to De Raeve, these conditions exist despite the high academic level of southern European nurses. In Portugal and Spain, there is a high training standard, so “you have a good and strong workforce and that is key,” he says. In contrast, Germany, which has more nurses, requires fewer qualifications of its nurses.
These differences may also explain why many southern European nurses packed their bags years ago to work in other regions. According to data published in the United Kingdom, almost 6% of the nurses in its national health system, some 19,325 nurses, come from other European countries. 60% of those come from Ireland, Portugal, Spain and Italy. The SATSE union points out that, according to estimates from years ago, more than 5,000 Spanish nurses may have gone to work in other regions, while, in the case of Italy, FNOPI estimates the number may be 20,000.
Nurses now face the fear of outbreaks and the return of the virus.
“A resurgence would be much worse. There is so much physical and mental exhaustion that we could not give the same effort no matter how much we wanted to,” García says.
For now, nurses remain in the breach, carrying out their usual duties and, in many regions, also taking charge of taking samples for testing or contact tracing, says Rocha, the CODEM spokesperson. Meanwhile, they are asking to work with more protection, better working conditions and the support of psychology specialists who can help them and other health workers to recover physically and emotionally from what happened.
“Since we have had this unfortunate situation, we ask that it not be forgotten and that we succeed in getting a strengthened healthcare system that revolves around the needs of patients,” García says.
That would convert the eight o’ clock applause into a new bulwark against future pandemics.
 This article is part of the European Data Journalism Network and it is published under a CC BY-SA 4.0 license.
This article is part of the European Data Journalism Network and it is published under a CC BY-SA 4.0 license.
Methodology
Data from this article is available for download here. Doctors and nurses per capita data are from Eurostat: in most cases, the figures are from 2017, although in Belgium, Denmark and Sweden, the numbers go back to 2016, and in Finland to 2014. In all cases, we compared the categories of practicing doctors and practicing nurses in each country.
In some countries, the figures for practicing nurses are overestimated: Austria and Latvia include nursing assistants, while Cyprus and Spain count midwives. Despite the fact midwives in Cyprus and Spain earn nursing degrees before specialising in obstetric and gynaecological care, the vast majority of European countries publish separate figures for midwives. Other countries could be reporting artificially low figures. For example, Czechia and Hungary do not count nurses working in care homes, Estonia does not include nurses specialised in radiology, Malta does not count self-employed nurses, Poland does not include prison nurses and the UK only reports public sector data.
In the case of doctors, some countries exclude certain specialities. Luxembourg, for example, excludes haematologists, microbiologists and pathologists, Germany excludes maxillofacial surgeons and Belgium excludes internal medicine doctors.
In addition, Italy estimates the number of practicing nurses using the register of professionals who have completed mandatory recurrent training in recent years. Finland’s estimate is based on a survey conducted in 2014 so their data may no longer be accurate. Finally, we have not included France, Portugal, Ireland and Slovakia since they do not publish their updated figures in Eurostat and the numbers that they report at national level and to the OECD do not correspond to the OECD category of practicing professionals, for doctors and nurses. We have also decided to exclude Romania, given that its numbers for nurses include workers such as laboratory assistants and forensic assistants, among others.
To calculate the ratio of nurses to doctors, we used the total doctors and nurses by country data published by Eurostat, not the per capita figures. We did not include Greece and the Czechia in the ratio calculation since their medical personnel data are inconsistent.